You know how it goes. You get sick—a nasty flu, a bad cold, maybe something more exotic. You ride out the fever, the aches, the fatigue. After a week or two, you expect to bounce back. To be you again.
But for a significant number of people, that bounce back never fully happens. The virus leaves, but the shadow of it lingers. For years, we’ve talked about this in the context of a few conditions, like myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) or the neurological aftermath of mononucleosis. But honestly, that’s just the tip of the iceberg.
Post-viral syndromes are a vast, often misunderstood frontier in medicine. They represent a collection of long-term symptoms that persist long after the initial infection has cleared. And they can be triggered by a whole host of viruses—not just the famous ones.
Beyond the Usual Suspects: A Wider Viral Landscape
Sure, we’ve all heard of “long COVID.” It’s the post-viral condition that, frankly, forced the conversation into the mainstream. But it’s far from alone. The medical history books—and countless patient forums—are filled with stories of people whose lives were quietly upended by other viruses.
Think about Epstein-Barr virus (EBV). For most, it’s a teenage rite of passage. For some, it’s the starting pistol for decades of debilitating fatigue and brain fog. Or enteroviruses, which have been linked to everything from persistent muscle weakness to heart complications. Even common rhinoviruses (the typical cold virus) have been implicated in triggering long-term issues for a subset of people.
The pattern is the unsettling part: a clear infection, a recovery that plateaus or stalls, and then a new, chronic normal sets in. The virus itself might be gone, but it’s like it flipped a switch in the body’s complex operating system—a switch that’s notoriously hard to flip back.
What Does a Post-Viral Syndrome Actually Feel Like?
Imagine your body’s battery no longer charges to 100%. Maybe it tops out at 45% on a good day. That’s the energy piece. But the symptoms are a kaleidoscope, often overlapping in frustrating ways.
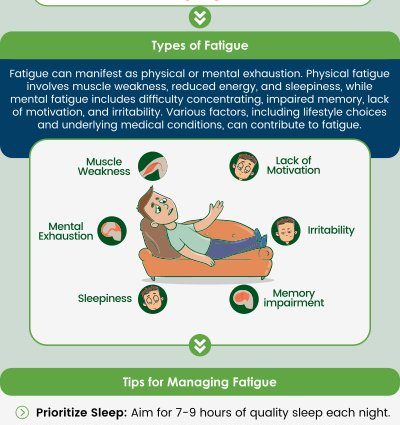
- Crushing Fatigue: Not just “I need a nap” tired. This is a deep, bone-weary exhaustion that isn’t relieved by sleep and is often made worse by minor physical or mental exertion. Patients call it “post-exertional malaise” (PEM), and it’s a hallmark.
- Brain Fog: Your thoughts move through molasses. Finding words, concentrating, remembering simple details—it all becomes a struggle. It’s like the cognitive equivalent of a blurry, buffering video.
- Widespread Pain: Unexplained muscle aches, joint pain, or nerve pain (like tingling or burning) that migrates and often defies easy diagnosis.
- Autonomic Dysfunction: This is a big one. The virus seems to disrupt the autonomic nervous system—the automatic pilot that controls heart rate, blood pressure, and digestion. This leads to dizziness, rapid heartbeat (POTS), and gut issues.
The real kicker? These symptoms are often “invisible.” Blood tests come back normal. Scans show nothing obvious. Which, sadly, has led to a long history of patients being dismissed or told it’s “all in their head.”
The Body in Rebellion: Possible Mechanisms at Play
So what’s actually happening? Why does the body keep fighting a war the virus has already left? Researchers are piecing together a few compelling theories—it’s rarely just one thing.
1. The Immune System Gets Stuck “On”
One leading idea is viral persistence. Fragments of the virus might hide in tissues, continuously tickling the immune system into a low-grade, chronic state of inflammation. It’s like having a fire alarm that won’t turn off because there’s still a tiny, smoldering ember somewhere in the walls.
2. Autoimmunity: Friendly Fire
Sometimes, in its zeal to attack the virus, the immune system gets confused. It starts making antibodies that attack the body’s own tissues—a case of mistaken identity. This “autoimmune” response can damage nerves, joints, or glands, creating lasting symptoms.
3. Cellular Energy Crisis
Mitochondria are the tiny power plants in our cells. Some research suggests certain viruses can damage them or disrupt how they function. If your cellular power plants are broken, you’re going to feel it everywhere—as profound fatigue and poor recovery.
Navigating Diagnosis and the Path to Management
Let’s be real: getting a diagnosis for a poorly understood post-viral condition is often an uphill battle. There’s no single test. It’s a process of elimination, a detailed patient history, and finding a clinician who listens.
That said, the approach is becoming more standardized, thanks in part to the focus on long COVID. A good workup might involve:
| System Checked | Possible Tests/Assessments |
| Immune & Inflammatory | CRP, ESR, Autoantibody panels |
| Autonomic Nervous System | Tilt-table test for POTS, heart rate variability |
| Metabolic & Mitochondrial | Basic metabolic panel, CPET (exercise test)* |
| Neurological/Cognitive | Neuropsychological evaluation, brain MRI |
*Done with extreme caution to avoid post-exertional crash.
Management, for now, is less about cure and more about careful, personalized symptom management. Think of it as re-learning how to live within your body’s new energy envelope. Pacing activity is crucial—learning to stop before you hit the wall. Diet modifications, gentle graded exercise (when appropriate), sleep hygiene, and treating specific symptoms like pain or dizziness form the cornerstone.
A New Chapter in Medicine
Here’s the deal: the massive scale of long COVID has ripped the blindfold off the medical community. It’s proving, undeniably, that post-viral syndromes are real, complex, and devastatingly common. The research pouring into long COVID isn’t just for one disease—it’s illuminating a whole dark corner of medicine that has affected people for generations.
We’re starting to ask better questions. To connect the dots between different post-viral conditions. The goal? To move from just managing symptoms to understanding the root causes—and eventually, to finding ways to reset that switched-off system.
For anyone living in the long shadow of a virus, that shift in understanding might be the most important symptom of all: hope.